Headache is the most commonly reported symptom after whiplash injury, but the exact source of headache is a matter of controversy. Some have speculated that headache may be caused by post-concussion syndrome or by mild head injury, but researchers have had difficulty identifying the lesion responsible for such an injury. A more accepted source of headache is the cervical spine—what is known as cervicogenic headache.
Researchers from Ohio1 have performed an anatomical study that lends credence to the notion of cervicogenic headache—specifically, headache arising from entrapment of the C2 nerve root ganglion. Fifteen cadaveric spines were examined, and the authors measured the height of the foramen and the height of the ganglion.
The authors found that the C2 ganglion occupies, on average, 76% of the space provided by the foramen. The illustration shows the atlas, axis, and C2 nerve root ganglion:
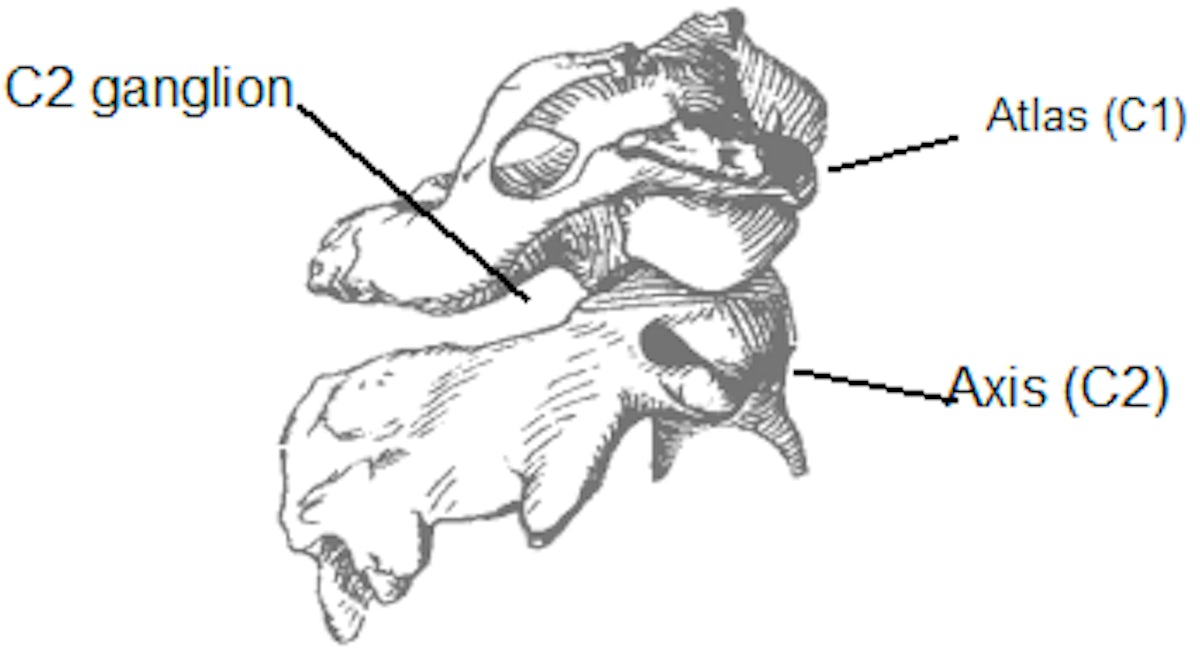
From their anatomical findings, the researchers suggest that the C2 ganglion is particularly susceptible to compression, resulting in damage to the nerve and headache.
"Considering these results, the authors believe that the anatomic features of C2 ganglion may predispose to its vulnerability to compression. In the report of his cadaveric study, Bogduk2 noted that during rotation combined with extension (i.e., whiplash injury), the posterior arch of the atlas and the superior articular process of the axis were approximated sufficiently to contact the C2 ganglion. The C2 ganglion, the thickest neural structure, is the most susceptible to compression."
The authors further state that, "It is likely, therefore, that the cervicogenic headache occurs as a result of displacement, abnormal movements, or arthritic changes in the atlantoaxial joint where the C2 ganglion and nerve root are compromised."
- Lu J, Ebraheim NA. Anatomic considerations of C2 nerve root ganglion. Spine 1998;23(6):649-652.
- Bogduk N. The anatomy of occipital neuralgia. Clinical and Experimental Neurology 1981;17:167-184.